
Dr Ian Marr from the Canberra Hospital’s Infectious Disease Unit has done a lot of work on the Buruli ulcer, Photo: James Coleman.
Work is continuing to determine why there’s been a spike in cases of flesh-eating, mosquito-borne infection across Australia’s southeast.
The bad news? Researchers are still baffled.
However, we met up with Canberra Hospital’s infectious disease unit director and clinical microbiologist, Dr Ian Marr, to find out what we know so far about the dreaded ‘Buruli ulcer’.
Dr Marr is among a group of researchers from Canberra Health Services, the Doherty Institute, the University of Wollongong, NSW Health and Austin Health who published a paper on it after two cases were reported in Batemans Bay in 2023 – the first for the area in a decade.
He also investigated the first case that presented to the Canberra Hospital in 2023, which involved an elderly man who had caught his finger in an outdoor chair while holidaying on the South Coast.
“He’d gone onto to have this in-grated lesion and breakdown of his finger some months later,” Dr Marr says.
“It was a challenging diagnosis to make, but after a number of weeks, we were able to secure the diagnosis.”
What is the Buruli ulcer?
The Buruli ulcer’s full name is ‘Mycobacterium ulcerans infection’.
According to the World Health Organisation (WHO), it is a “chronic debilitating disease” found in at least 33 countries with tropical, subtropical and temperate climates (Africa, South America and the West Pacific, including Australia).
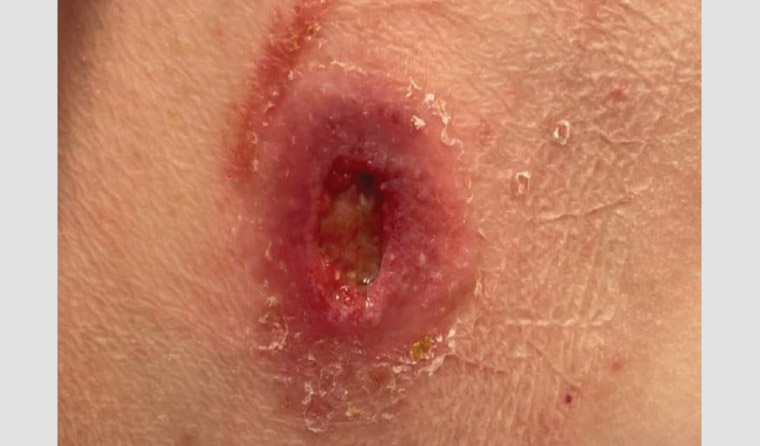
Buruli ulcer. The ulcer may only form up to five months after the bite, so there’s a long incubation period. Photo: Royal Australian College of General Practitioners.
What starts as a painless swelling will progress into an ulcer within about five months, which – left untreated – “can lead to permanent disfigurement and long-term disability”.
Where does it come from?
“So Mycobacterium ulcerans – and this is new information as of last year – actually proliferates in certain mammals, and possums are thought to be what we call the amplifying hosts,” Dr Marr explains.
“That means the mycobacterium sits in the possum and can grow in number into a large number, infect them, and cause ulcerative lesions in the possums.
“And then mosquitoes look like the vector, so they’re able to take it from the possum and then transfer it across to humans in the form of a bite.”
The first case was reported in Uganda in the 1940s by a British surgeon who found “disfiguring skin lesions on a number of people in a village he had been working in”.

Dr Marr says the next step in research involves working out how to decrease the spread of the bacteria among possums. Photo: James Coleman.
Since then, it’s been reported here in Australia in parts of Queensland, Northern Territory, and – most often – Victoria, where the number of cases has steadily increased to between about 200 and 360 cases every year since 2017.
The disease popped up for the first time in Southern NSW in 2021, followed by the two cases near Batemans Bay in 2023.
This month, the Southern NSW Local Health District issued a warning to residents following a fourth case – the first in two years.
So far, in Australia, cases have been limited to coastal areas – but researchers aren’t sure why.
“There are certain thoughts, but no one’s been able to definitively prove any of their hypotheses as to why that is the case,” Dr Marr says.
Most of the work at the moment is directed at preventing the spread using DNA-tracking of the bacteria to work out where it’s been.
“Melbourne’s Doherty Institute has done some terrific work on their genome sequencing of the bacterium where they’ve looked inside the DNA and been able to unpack that and find out where it’s come from,” he says.
This is what has led them to believe possums are to blame, so a lot of the latest research is about “trying to understand if we can cut off those vectors and decrease the number of mosquitoes in an area or what we can to do limit it terms of the possums as well”.
How do you know if you’ve got it?
“An ongoing painless ulcer is one of the things you really want to pay attention to,” Dr Marr says.
The ulcer may only form up to five months after the bite, so there’s a long incubation period, too.
“Just get a swab onto that – your GP should be able to get that. That can be sent off to laboratories in Sydney and Melbourne, and they can test it using the PCR method, similar to how COVID is tested.”

The Canberra Hospital is among several institutions around the country investigating the infection. Photo: James Coleman.
What happens if I do get it?
You’ll be relieved to hear that the cure has improved since the 1940s.
“There were certain surgical techniques that were used to cut it out, but with the advent and discovery of more and more antibiotics, we’re able to treat this with two types of antibiotic pills over eight weeks, sometimes a little bit longer.
“It kills the bacterium, and the skin heals back.”
Is there anything I can do now?
For now, Dr Marr says there is no other advice other than to “avoid mosquitoes as much as possible”.
“Wear anti-mosquito repellent, wear long sleeves, wear long pants, especially in the evenings and early mornings.”















